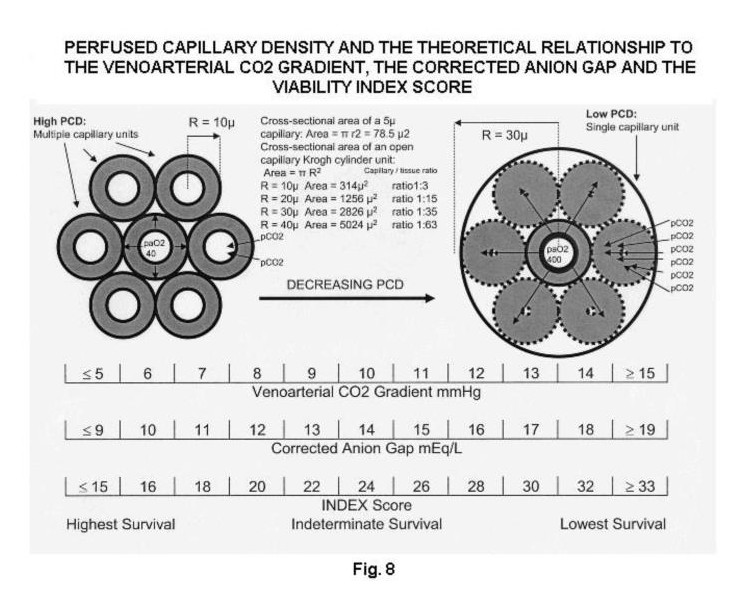
The theoretical relationship between perfused capillary density (PCD), the venoarterial CO2 gradient, the corrected anion gap and the Viability Index Score.
Survival is dependent on maintaining adequate PCD within vital tissues and organs. As long as PCD remains high, the ability to exchange oxygen and carbon dioxide at the microvascular level remains adequate even if the factors governing the Fick principle are sub-optimal. However a patient with a low PCD is at high risk of mortality even if oxygen delivery and hemodynamics are within the normal range. This figure illustrates the theoretical relationship between PCD, the AGc, the p[v-a]CO2 and the Viability Index. Each of the components of the Viability Index (the AGc and the p[v-a]CO2) is an important assessment tool by itself. By combining the components together to create a VI score the assessment value improves. For example, a p[v-a]CO2 of 6 mmHg and a AGc of 10 mEq/L each predict high survival and theoretical correlation to high PCD. A p[v-a]CO2 of 14 mmHg and a AGc of 18 mEq/L each predict poor survival and a theoretical correlation to low PCD.
But what assessment can be made if the p[v-a]CO2 is 6 mmHg and the AGc is 18 mEq/L? The resultant VI score of 24 would indicate an indeterminate survival of only about 50% and the need for more effective intervention. What assessment can be made if the p[v-a]CO2 is 14 mmHg and the AGc is 10 mEq/L ? Again the resultant VI score of 24 would indicate that more effective treatment is necessary.

Perfusion Theory is an educational platform for the Oxygen Pressure Field Theory (OPFT). August Krogh’s theoretical concept of the oxygen pressure field is explained and then applied to clinical applications in perfusion practice.