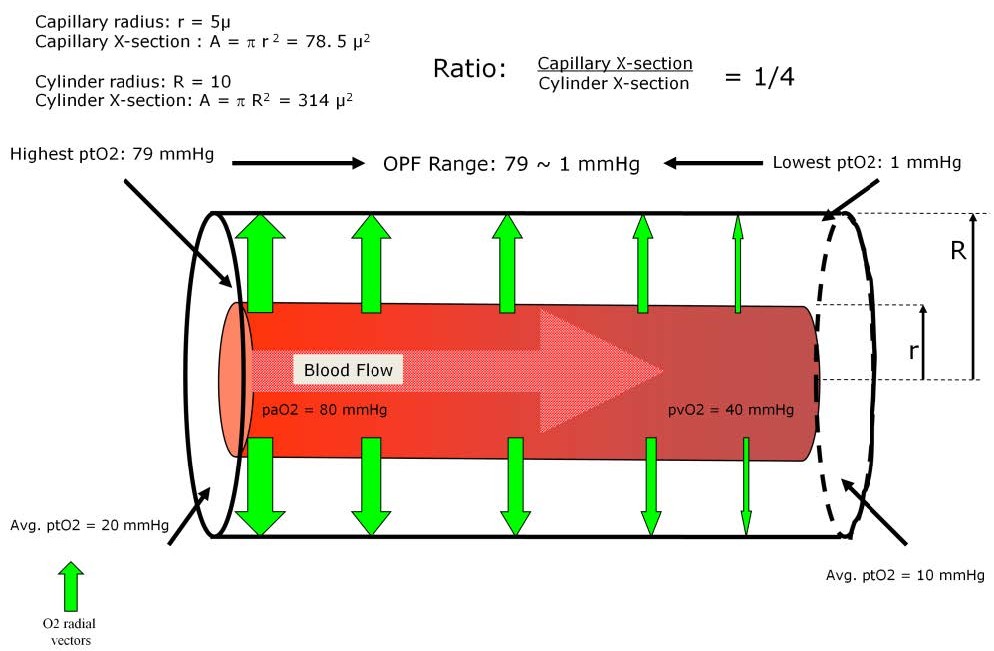
Diagram example of the fundamental concept of the Krogh cylinder and the oxygen pressure field values.
The Krogh cylinder model is a simple way to describe an oxygen pressure field. Dr. Krogh envisioned a capillary surrounded by a sleeve of tissue to which the capillary provided gas exchange and nutrients. The tissue cylinder pictured here as an example has a capillary radius of 5 microns (μ) and a cylinder radius of 10 μ. This results in a capillary-to-cylinder cross-sectional area and volume relationship of 1:4. As blood enters the capillary the oxygen leaves the hemoglobin to expand out of the capillary and into the cylinder volume made up of the living tissues. In this example, the arterial pO2 value of the blood entering the capillary remains steady at 80 mmHg. The oxygen will expand into the arterial-end tissues of the cylinder resulting in a stable average tissue pO2 of 20 mmHg. At the venous end of the cylinder the intracapillary pO2 of the blood has fallen to 40 mmHg and after expanding into the cylinder volume the average tissue pO2 will be 10 mmHg.
At the arterial end of the cylinder and near the capillary itself the tissue pO2 may be almost equal to the arterial pO2 of the blood (79 mmHg). At the venous end of the cylinder and farthest from the capillary the tissue pO2 may approach zero (1 mmHg). The oxygen pressure field in the tissues around this capillary has a range of 79 mmHg to 1 mmHg. The median value would be approximately 20 mmHg, meaning that 50% of the tissues have pO2 values greater than 20 mmHg and 50% have values less than 20 mmHg.
The oxygen unloads from the capillary blood and follows radial vectors to enter the tissue. Radial vectors move at right angles to the capillary axis. The strength of the vectors (gradient) depends upon the intracapillary pO2 value and the tissue pO2 value. At the arterial end the capillary pO2 is 80 mmHg and the tissue pO2 is 20 mmHg; the gradient would be 60 mmHg. At the venous end the capillary pO2 is 40 mmHg and the tissue pO2 is 10 mmHg; the gradient would be only 30 mmHg. This means that more O2 will move into the cylinder at a faster rate at the arterial end than at the venous end of the cylinder. The values shown here are not absolute but serve only as examples.

Perfusion Theory is an educational platform for the Oxygen Pressure Field Theory (OPFT). August Krogh’s theoretical concept of the oxygen pressure field is explained and then applied to clinical applications in perfusion practice.