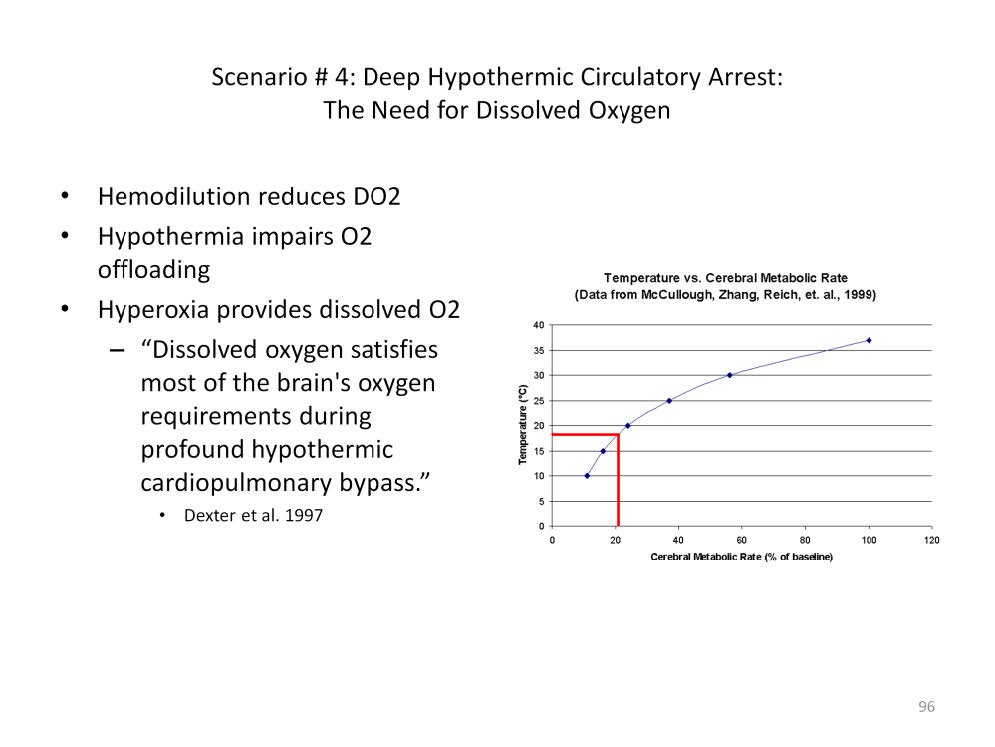
As the body and blood are cooled during CPB, the metabolic rate is reduced. At 18° C the metabolic rate is thought to be about 10% of normal. However experiments have shown that cerebral metabolism is considerably higher at 18° C than once thought. Other problems complicate the cooling process. Hemodilution reduces oxygen delivery. Hypothermia impairs the release of oxygen from the remaining oxyhemoglobin. The p50 indicates the ability of the hemoglobin to release oxygen in relation to the tissue oxygen concentration. At 37° C, the p50 of hemoglobin is 27 mmHg and the average tissue pO2 is also about 27 mmHg. At 18° C, the p50 is only about 7 mmHg, meaning that the tissue pO2 value must fall to an average of 7 mmHg to force the transfer of oxygen from the hemoglobin to the tissues. The reduction in CO2 production further reduces the release of oxygen from the blood. Hemoglobin becomes essentially nonfunctional for oxygen exchange at profound temperatures unless the tissue oxygen concentration drops to extremely low levels.
However as blood cools, oxygen becomes more soluble. Once the hemoglobin is fully saturated a considerable amount of dissolved oxygen can be carried by the blood if it is exposed to a high FiO2 sweep gas. Dissolved oxygen is not limited by the effects of cold hemoglobin and is therefore available to any needy tissues.

Perfusion Theory is an educational platform for the Oxygen Pressure Field Theory (OPFT). August Krogh’s theoretical concept of the oxygen pressure field is explained and then applied to clinical applications in perfusion practice.